Early Concussion
-
Stage One 24-48 hours
-
Stage Two
-
Stage Three
Stage One 24 to 48 hours
- See your GP or a trained healthcare professional for review.
- The main symptoms you will likely need to manage are headaches, dizziness and nausea.
- For the first 24-hours, be monitored for red flags by a responsible adult.
- Reduced activity is recommended for the first 24-48 hours. Avoid complete rest, most activities of daily living can resume immediately.
- Prioritize a restful night’s sleep, regular healthy snacks, and plenty of water.
- Minimize screen time (this includes TV, computers, phone, gaming).
- Avoid alcohol, drugs, driving, air travel, strenuous exercise, and operating heavy machinery.
- Use pain relief as required for headaches.
- Speak to your GP should a medical certificate be required to enable you to take time off work initially.
Resources
Headaches
Headaches are a very common symptom post-concussion following impact to the head and neck. There are many different types of headaches that may occur, and an assessment by an appropriately trained health professional will assist in identifying the likely cause and best management.
Strategies to manage headaches
- Simple analgesics (NSAIDS and paracetamol).
- Maintain consistent bedtime and wake time.
- Manage triggers where possible (i.e. screen time, neck position when using screens).
- Consuming consistent meals (no delayed or skipped meals) and adequate hydration.
- Regular low-intensity cardiovascular exercise (i.e. walking), progressing slowly as symptoms allow.
- Use of relaxation strategies (i.e. mindfulness-based strategies) and stress management.
- Review of personal, environmental, work / school related and physical factors should be identified and addresses as potential headache contributors.
- Use a headache diary to track your symptoms and assist with diagnosis of cause (please see example below).
Components tracked in a headache diary |
|||||
| Date | Time (start / finish) | Preceding symptoms | Triggers | Medication (and dosage) or management | Relief (complete, moderate, none) |
|---|---|---|---|---|---|
Dizziness
Dizziness, balance and visual problems are very common after a concussion. These problems can occur for several reasons including injury to the neck, vestibular and oculomotor systems. It is important to establish which system/s is impaired to ensure the best recovery and adequate treatment is provided.
Issues with persistent vertigo (a sense that you or your surroundings are spinning), reduced balance, dizziness and visual instability are often symptoms associated with vestibular impairment. The vestibular system helps us to keep our balance, maintain posture and stabilise our head and body during movement. Vestibular issues are common after trauma to the head and can delay concussion recovery.
Depending on the type of vestibular impairment, different treatment interventions will be recommended. Your symptoms can be assessed by a health professional with further training in this area. Initial tests are often completed by a GP or physiotherapist but may also require referral to other health professionals. Your health professional may look at your balance, coordination, vestibular system, vision and hearing.
Neck symptoms
Symptoms following concussion are not always specific to brain injury. Movement forces to the head and neck at the time of concussion can result in injury to the cervical spine (neck) and supporting muscles. The neck plays an important role in giving feedback about where the head is in space and sensors in our neck also help the visual and vestibular (balance) systems. Given these connections, ongoing symptoms such as dizziness, headache, blurred vision, vertigo and poor concentration can occur from both prolonged post-concussion symptoms or due to a cervicogenic / neck injury.
Once a more severe injury (i.e. fracture) is ruled out, returning to normal movement and graded activity post injury is important to help the neck recover. Completing gentle range of movement neck exercises can assist in returning the normal and controlled movement to the neck post injury. This can minimise ongoing symptoms, including stiffness, tension and pain.
With ongoing symptoms, you may notice you change the way you move and / or hold your head after an injury (e.g. turning your whole body to turn your head instead of just turning at the neck, holding your head off to one side or even holding tension in your neck muscles by bringing your shoulders up to your ears). These examples are often protective or compensatory habits. If you notice you are doing these things, try to:
- Return to normal movement by resetting your head position and posture.
- Relax any muscles with tension (e.g. dropping your shoulders)
- Complete gentle range of movement neck exercises to help build control and support around the area.
If you have ongoing cervicogenic / neck issues, a review by a musculoskeletal physiotherapist is recommended to further examine and treat ongoing issues. If there are signs of ongoing or progressive headaches, weakness, tingling, numbness or severe pain, a GP or a medical review is recommended.
Hearing symptoms
Not all your symptoms may be a direct result of concussion. An injury that causes concussion can also cause trauma to other parts of the body, including the middle and inner ear areas that are commonly affected by a force to the head. As a result, you may have a mix of concussion and ear-related symptoms.
Ear symptoms can include:
- Loss of hearing in one or both ears
- Noises or ringing in the ears or head (tinnitus)
- Loss of balance, dizziness or understanding of position in space
- Sense of pressure, fullness or pain in one or both ears
- Clear discharge or bleeding from the ear canal
- Dizziness triggered by loud noises, sneezing or coughing (semicircular canal dehiscence or SCCD)
- Loud internal body noises of own voice, chewing, footsteps or eye movements (autophony) (also SCCD).
It is important to know what is causing these symptoms so that you can receive the correct advice for management. The ear related symptoms (hearing, ear pressure, fullness and tinnitus) can be referred to an audiologist initially and symptoms such as discharge and vertigo to ENT (Ear, Nose and Throat) specialist doctor. You may need to see both specialists.
Stage Two (Home)
As your post-concussion symptoms improve, you will need to:
- Attempt short amounts of activity around the home
- Slowly increase exercise to gradually get your heart rate up
- Take regular breaks to refresh yourself
- Continue regular food, water, sleep and symptom-specific medication (if still needed)
- Keep stress levels and demands low
- Gradually desensitize your intolerances to noise, light, and movement
- Optimise sleep hygiene
If your symptoms of headache, nausea or dizziness worsen after activity, then you need to take a break. Then reduce your activity and expectations of what you can achieve by about 20%.
Some people describe this as the “brain fog” stage. Brain fog includes trouble concentrating, slowness in thinking or difficulty remembering and learning new information.
Resources
Noise and light sensitivity
After sustaining a concussion, it can be common to:
- Want to spend time in a dark room, with no demands.
- Find loud, high-pitched or abrasive noises overwhelming.
- Find sunlight and bright technology screens overwhelming.
Noise or light sensitivity can also make other symptoms such as headaches, nausea and dizziness worse.
An initial period of relative rest is recommended the first 24 to 48 hours. Following this, people experiencing sensory sensitivity are encouraged to engage in activities that only mildly worsen symptoms (i.e. no worse than a 2-point increase in symptoms from baseline symptoms, on a scale ranging from 0 to 10), as long as the symptoms return to baseline shortly afterward.
How to gradually desensitize to these intolerances:
- Short term usage of noise cancelling headphones or ear plugs.
- Reduced screen brightness or enable night-mode on devices, as well as reduced screen time (this includes phones, computers and TV).
- Alter your environment as needed initially – blinds down / dimmed lights during the day, limit background noise, use of a hat and sunglasses outdoors.
- Turn volume down on TV / computer.
Eating habits
There is currently limited literature in this area; the following information is based on client experience and expertise of healthcare practitioners:
- Eating a nutritious and balanced diet is doubly important while your brain heals from concussion. Consider limiting high-sugar foods and junk food.
- Eat regular snacks or small meals throughout the day to maintain energy levels.
- Timers / alarms on your phone / watch can help with prompting regular eating.
- Limit alcohol and coffee, as stimulants impact on sleep cycle as well as potentially exacerbating symptoms of fatigue and dizziness.
- GP and / or dietician may assist with establishing a more consistent diet.
Vision
- Visual symptoms you may experience following a concussion include blurred vision, double vision, light sensitivity, difficulty reading, and headache and fatigue following visual activities (such as reading or in complex visual environments such as the supermarket). This may be due to effects on the brain’s ability to control focusing and eye coordination following a concussion.
- If visual changes are noted, it may be appropriate to see an optometrist who specialises in neurological conditions, also known as a neuro-optometrist. They can accurately assess the vision problems to determine what is causing the symptoms. Treatments may include spectacle lenses, prisms, tinted lenses, or vision therapy if indicated. Your eye health will be assessed as part of the comprehensive assessment.
Cognitive changes
You can have cognitive changes to your thinking and memory following a concussion. Common cognitive issues after concussion are observed in the domains of attention / concentration, processing speed, memory and learning, and executive functions (e.g., initiation, task-monitoring, planning / organisation). Difficulties are most pronounced in the acute phase of concussion (i.e., 48 hours post-injury), but may persist for several weeks. In most cases, full cognitive recovery is expected within one month.
To assist with an effective cognitive recovery, it is generally most important to:
- Acknowledge that cognitive changes are temporary
- Aim for a slow, progressive return to your previous level of cognitive functioning
- Use appropriate strategies to support your recovery
Attention and Cconcentration
- Give yourself longer to react to and process the information
- Read for shorter periods; limit how much you can view when reading (for example, covering sections on a page of writing, or enlarging a window on a computer screen)
- Reduce distractions; use earplugs, white noise, and/or work in a quiet room with the door shut
Memory
- Repeat/rehearse information out loud to aid memory
- Use visual tools and cues e.g. Post-it notes; reminder lists
- Write things down – research shows this can help consolidate the information into memory stores
Initiation and monitoring (starting and completing tasks)
- Use alarms and diaries to prompt you to start or change activity
- Complete one task at a time
Planning / organisation
- Use a calendar
- Make a daily to-do list
- Break tasks down into “urgent”, “important”, and “non-urgent”
- Declutter your home and office to reduce visual scanning demands
Using computers and phones
If you are continuing to struggle with reading and writing on the computer or phone, then some software adaptations may help to make this easier.
Some options are listed below:
- Dictate function in Microsoft Word
- You can type and edit by speaking in Google Docs or in Google Slides speaker notes
- Siri can be used to send text and read messages for Apple devices
- Read & Write software does text-to-speech and speech-to-text for Windows, Mac, Google Chrome, Microsoft Edge, iPad and Android
- Otter.ai is an app that records meetings, takes notes in real time and generates an automated summary
- Speechify allows you to read web pages, PDFs and Google Docs
- Sonocent helps with note taking for lectures and tutorials, on Apple, Windows, and mobile phones
- C-Pen can read out loud printed documents, you scroll over
- Audiobooks can be setup on your iPad or Android device to reduce visual processing.
Fatigue
Fatigue is common while your brain is recovering from the concussion. Fatigue may also be influenced by other factors such as sleep, mood, nutrition, metabolic factors e.g. anaemia.
Fatigue may be:
- Cognitive – getting tired from concentrating, multi-tasking, time pressures, and complex thinking
- Physical – getting tired from physical activity and exercise
- Emotional – getting tired from personal interactions, relationship changes or stressors
After a brief period of rest during the acute phase (24 to 48 hours), a gradual return to usual activity is recommended based on your tolerances. Some people find that some symptoms may be more noticeable when fatigued e.g. headaches develop, difficulty with memory, or feeling overwhelmed. Fatigue is often well managed through planning, pacing, taking regular breaks, and healthy lifestyle factors.
Strategies for managing fatigue:
- Sleep well and wake refreshed (reduce naps if affecting your night’s sleep)
- Regular light exercise to help you feel positive and energised
- No alcohol or illicit drugs that can affect your mood, reactions, and hydration
- Eat a healthy diet. Consider smaller more regular meals
- Learn stress management techniques, to deal better with stress and pressure.
- Limit caffeine/energy drinks/sugar as they provide a false expectation of your body’s energy
Exercise and activity post-concussion
The best way to assist the body to regulate itself again post-concussion is through a graded return to activity.
- After the initial 24 to 48 hours relative rest period, it is important to resume gentle activity and movement. This helps give gentle exposure to external environments (e.g. lights, noise, movement) and can help with mood and mental health.
Doing too little initially or pushing too much too soon can delay recovery.
- Post-concussion, the body’s autonomic nervous system regulation can be impacted. The autonomic nervous system is responsible for regulating key involuntary functions including heart rate, blood pressure, breathing, digestion and gland secretion.
- Too little: The body needs some regular activity to gently challenge these systems and promote normal regulation. Extended rest leads to deconditioning (losing fitness) which can mean easier irritation of symptoms and can prolong symptoms such as fatigue, sleep disturbance and irritability.
- Too much: If pushed too hard too early you may get irritation of your symptoms (e.g. headache, dizziness or fogginess) as the systems get overloaded and struggle to regulate themselves.
The aim is to find the sweet spot doing as much as you can with minimal symptoms.
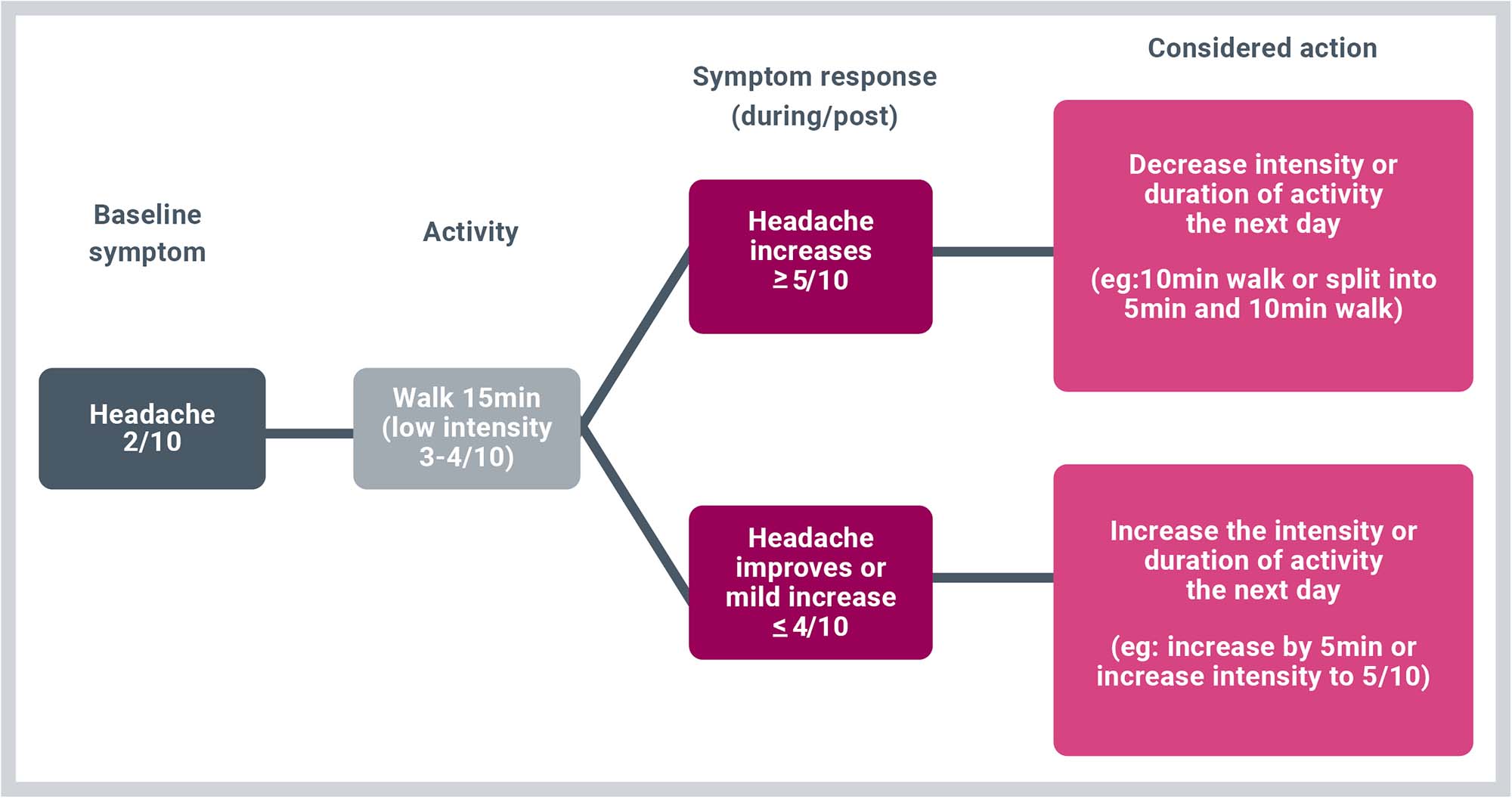
- As a general activity guide, initially aim for 15 to 20 minutes of gentle walking or low-grade cardio daily and gradually build from there. If this is too much at once, break into smaller timeframes throughout the day and gradually work up.
- It can be useful to score your symptoms on a 0 to10 scale prior to activity and consider the +3 rule
- If your score increases by 3 or more during the activity, the intensity or duration should be temporarily lowered to a manageable level.
- If your score increases by less than 3 or improves during activity, you can step up the intensity or duration the following day.
- If your symptoms at baseline are limiting you from participating in regular activity a review by your GP / healthcare provider is recommended to provide further guidance and enable you to return to activity.
If you continue to have ongoing symptoms and / or you are returning to sport or other high-level activities (e.g. manual labour, military duty) it is recommended you see a physiotherapist experienced with concussion to assess your readiness to return to your chosen activity. Trained therapists can assess your response to exertion using tests such as the Buffalo Concussion Treadmill Test (BCTT) and, based on these results, prescribe a tailored exercise program for you.
- For return to sports and higher-level activity, it is recommended you are reviewed by a healthcare practitioner as well as a physiotherapist with concussion experience if medically recommended. Following a confirmed concussion, return to sport is recommended to be delayed until you have been 14-days symptom free period, and not before 21 days after the injury.
Stage Three (Home and Community)
Gradual step ups are required to get back to your best functional level (physical, cognitive / mental and emotional). However, it is important to be aware that you may increase symptoms when you first attempt that step up, but the next time you challenge yourself in the same way you should feel it is getting easier. When experimenting with these step ups only change one thing at a time, so that you are more likely to identify the triggers for your symptoms.
You can now start setting more realistic goals and time frames for return to driving, work, study or sport. You can increase your exercise, but also consider if you had additional trauma / injury from the initial incident, this may also affect your ability to safely return to activities. You need to consider ongoing sensitivities (eg light / noise) and/or changes in function (eg balance) where you may need a different approach to manage returning to your usual activities. You also need to continue with the basics of:
- Regular food, water, and medication (if still required)
- Good sleep and breaks during the day.
If it has taken only a few weeks to move through these three stages, you will likely return to a regular life balance with no major changes. However, if your recovery process has taken you months, the information in Stage 4 will be more important for you.
Resources
Driving
There are no legal requirements regarding returning to driving following a concussion, as the expectation is that most people will return to all previous activities with little to no changes in performance within one to four weeks. If you have ongoing symptoms that may impact your ability to drive, discuss these with your GP.
Symptoms that my effect safe driving include:
- Reduced concentration
- Headaches and fatigue
- Dizziness
- Overstimulation from fast moving environment
- Poor visual tracking
Drivers may be liable under common law if they continue to drive knowing they have a condition that is likely to adversely affect safe driving (Ref: AusRoads Guidelines 2025).
Return to sport
The risk of complications from concussion is increased if a player is permitted to return to sport before they have fully recovered. It is important that athletes do not return to contact activities or competition, until they have been reviewed by a Healthcare Practitioner (recommended at day 3 to 4 and after being symptom free for 14 days) and fully recovered. The Australian Sports Commission have released Australian Concussion Guidelines for Youth and Community Sport (PDF).
Please see below a summary of the graded return to sport framework, and refer to your individual sporting club and code’s guidelines as well where applicable.

Return to study
Seek medical advice before returning to study. Complete absence from the school environment is generally not recommended. As a guide consider this progression:
| Stage | Functional exercise | Objective |
| 1. Minor cognitive activity at home | Short periods (5 to 15min) of cognitive activity. Eg. reading, conversations, screen-based activities. | Gradually manage an increase in activities with minimal symptoms. |
| 2. Moderate cognitive activity at home | Longer periods (20 to 30mins) of cognitive activity. Eg. homework, reading, conversations, screen-based activity | Increase cognitive stamina, self paced activity |
| 3.Gradual return to school |
Part day of school attendance with access to breaks throughout the day. Academic accommodations may be considered, eg. reduced workload, extra time, environmental adjustments, graded return to homework. Complete absence from the school environment for the more than one (1) week is not generally recommended. |
Re-entry into school environment with accommodations, with minimal increase to symptoms. |
| 4. Gradual return to school - full days |
Gradual increase to full day of school attendance. Accommodation for testing could be considered. Eg. exams, quizzes. |
Increase cognitive stamina whilst gradually decreasing accommodations with minimal symptoms. |
| 5. Full cognitive workload resumed | Full cognitive workload without accommocations. | Full return to school. |
Return to work
Seek medical advice before returning to work. Generally, return to work can be considered when:
- You can tolerate longer periods of cognitive and physical activity
- You have resumed your usual daily routines and activities whilst most of your symptoms have settled.
As a guide you can consider this progression:
| Stage | Functional exercise | Objective |
| 1. Minor cognitive activity and light aerobic exercise in / around home | Short periods (5 to 15mins) of cognitive activity (texting / reading / conversations), going for short walks, and completing simple home / community chores eg. laundry, walking the dog. | Gradually manage an increase in activities with minimal symptoms. |
| 2. Moderate cognitive / physical activity in the home and community | Longer periods (20 to 30mins) of cognitive activity (socialising / reading / TV) or home / community tasks eg. grocery shopping. | Increase cognitive / physical stamina, self paced activity. |
| 3.Gradual RTW | Consider 3 mornings a week (ie Monday, Wednesday, Friday) for 3 to 4 hours.Consider accommodations eg. quiet work environment, rest breaks, beginning on easier work duties, low time pressure, allowing increased time. | Gradually return to usual hours and duties as tolerated with minimal increase in symptoms. |
Mental health
People who have had a concussion are at increased risk for mental health difficulties. This is due to a number of processes:
- The autonomic nervous system (our fight/flight stress response) is often affected in injuries like a concussion. This means that you may experience increased anxiety, irritability, and increased stress levels while your brain recovers.
- While cognitive issues (i.e., problems with thinking skills and memory) are often mild, they still involve key functions, such as impulse control and emotional / behavioural regulation. Even mild impact on these core thinking skills can make it difficult to perform daily activities and to control your reactions to people or events.
- Symptoms such as thinking and memory difficulties, headaches, dizziness, nausea, and brain fog can make you want to withdraw from friends and family, cease work / study, and stop driving. Resting and reducing cognitive demands is beneficial in the short-term. However, prolonged disruption to everyday activities, especially social / leisure activities, can have a significant impact on mental health.
People with previous difficulties with managing anxiety, depression or other mental health problems may find that these problems become significantly exacerbated and are worsened after concussion.
Research shows that anxiety and depression, as well as sleep disturbance, are some of the strongest risk factors for “persisting post-concussive symptoms” (i.e., symptoms lasting longer than the typical one-month recovery period). This means that early treatment for mental health problems is extremely helpful in reducing post-concussive symptoms (e.g., attention/memory, fatigue, headaches, dizziness).
If you are experiencing symptoms of anxiety and/or depression, it is important to reach out to your GP for treatment. Your GP may also refer you to see a psychologist, a professional trained in the assessment of mental health issues. They may use a range of therapies as part of treatment. This includes evidence-based techniques, such as cognitive-behavioural therapy (CBT), and practical strategies designed to address your areas of concern, including lessening/alleviating mood symptoms, returning to social activity, and improving sleep and sleep hygiene.
More information on depression and anxiety can be found on the Beyond Blue website (external site)
Here are some other resources that may be helpful:
Contact us
Tel: (08) 6457 4488
Email: WAABIRS@health.wa.gov.au
Location: Ground Floor, E Block, Sir Charles Gairdner Hospital